Waking up with a throbbing pain in your head can ruin your entire day. For many, the immediate reaction is to reach for a painkiller and hope for the best. However, not all head pain is created equal. Understanding the difference between migraine and headache is the first step toward finding effective relief and reclaiming your quality of life. While a standard headache is often a temporary nuisance, a migraine is a complex neurological condition that requires a specialized approach to management. At Raj Hospitals, we believe that patient education is the foundation of effective healthcare. This guide will help you distinguish between these two common conditions, identify your triggers, and understand when it’s time to seek professional medical intervention.
What is a Headache?
A headache is generally defined as pain in the head or upper neck region. It occurs when the blood vessels, muscles, and nerves in the head are overstimulated or inflamed. Headaches vary significantly in intensity and duration, but they are typically categorized into two main types: primary and secondary. Primary headaches, such as tension headaches, are stand-alone conditions caused by overactivity of pain-sensitive structures in the head. Secondary headaches are symptoms of another underlying condition, such as a sinus infection, dehydration, or high blood pressure. Most people experience tension-type headaches, which feel like a tight band wrapping around the forehead. While uncomfortable, they rarely involve the debilitating sensory symptoms associated with migraines.
What is a Migraine?
A migraine is much more than just a “bad headache.” It is a primary neurological disorder characterized by recurrent attacks of moderate to severe pain. Unlike a standard headache, a migraine is often accompanied by a host of systemic symptoms. These can include nausea, vomiting, and extreme sensitivity to light, sound, or even certain smells. Migraines often occur in stages, starting with a “prodrome” phase (warning signs like mood changes) and sometimes including an “aura” (visual disturbances like flashing lights). The difference between migraine and headache lies in this complexity; a migraine affects the entire body’s sensory processing system, not just the localized muscles of the head.
Common Causes and Triggers
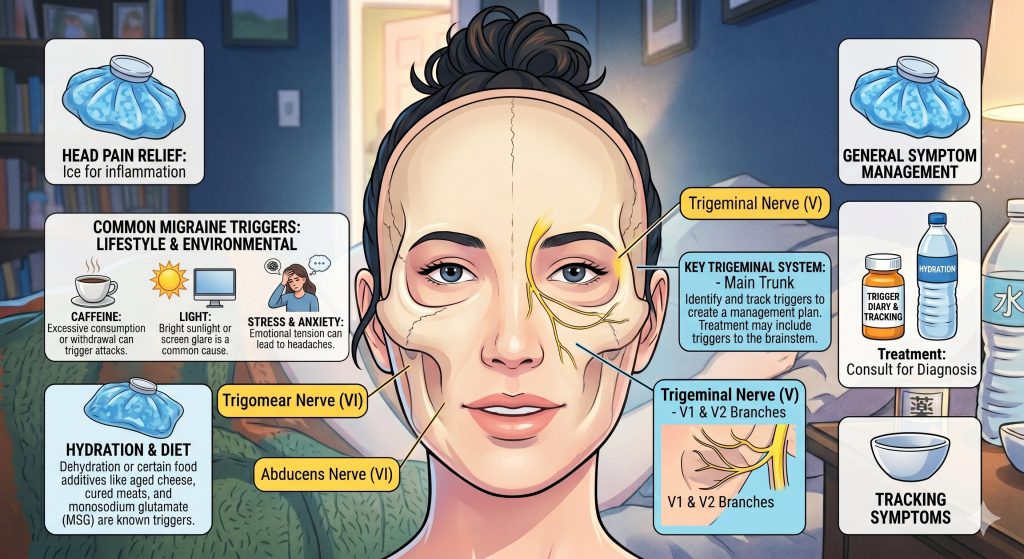
Understanding the root cause is essential for prevention. While the exact cause of migraines is still being researched, it is believed to involve genetic factors and changes in brain chemicals like serotonin.
- Stress and Anxiety: Emotional strain is a leading trigger for both tension headaches and migraines.
- Dietary Factors: Aged cheeses, salty foods, and processed meats containing nitrates can trigger attacks.
- Hormonal Changes: Many women notice a link between their menstrual cycle and the onset of migraines.
- Environmental Stimuli: Bright lights, sun glare, loud sounds, and strong odors (like perfume or smoke) are common culprits.
- Sleep Disruptions: Missing sleep or getting too much sleep can throw off the brain’s equilibrium.
- Physical Exertion: Intense physical activity may trigger symptoms in some individuals.
Symptoms: Spotting the Difference
Identifying the specific symptoms is the most reliable way to determine the difference between migraine and headache.
Headache Symptoms:
- Dull, aching sensation across the whole head.
- Pressure or tenderness around the forehead and scalp.
- Pain that usually lasts from 30 minutes to a few hours.
- No associated nausea or visual changes.
Migraine Symptoms:
- Intense pulsing or throbbing pain, often on one side of the head.
- Sensitivity to light (photophobia) and sound (phonophobia).
- Nausea and vomiting.
- Seeing “stars,” zigzag lines, or experiencing temporary vision loss (aura).
- Pain that can last anywhere from 4 to 72 hours if left untreated.
Comparing Migraine vs. Headache at a Glance
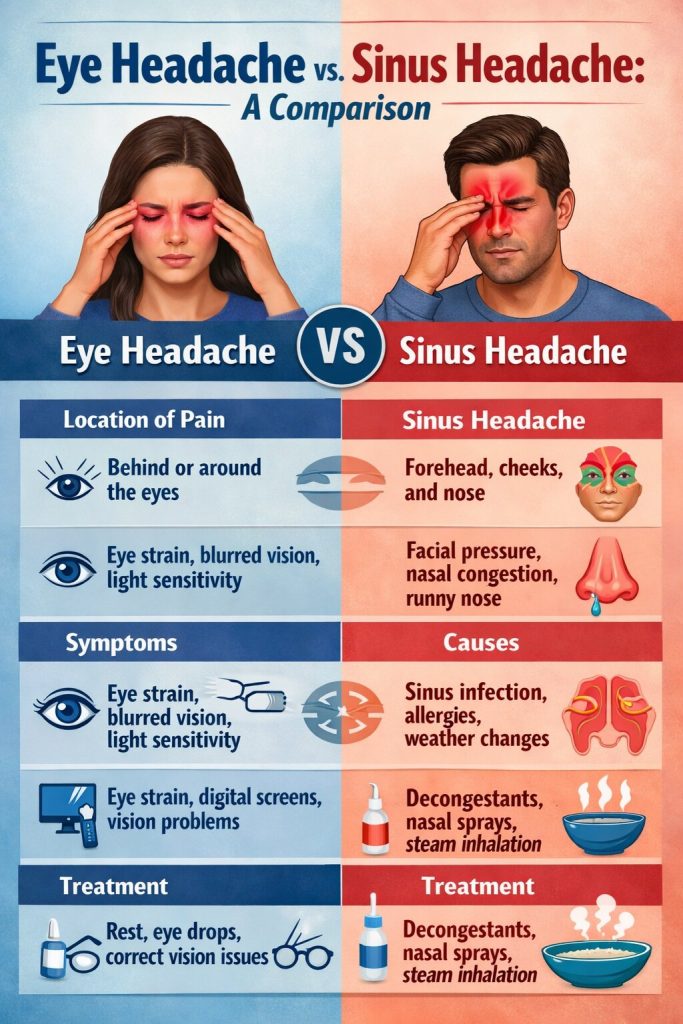
Diagnosis and Clinical Evaluation
If your head pain is frequent or interfering with your life, a clinical diagnosis is necessary. At Raj Hospitals, our neurology department utilizes a comprehensive approach to diagnosis. A doctor will review your medical history, frequency of attacks, and specific symptoms. In some cases, diagnostic imaging like an MRI or CT scan may be recommended to rule out secondary causes such as tumors or vascular issues. Keeping a “headache diary”—noting what you ate, your sleep patterns, and the weather before an attack—can be incredibly helpful for your specialist to identify patterns and provide an accurate diagnosis.
Treatment Options for Relief
Treating the difference between migraine and headache requires different strategies.
For Headaches:
Most tension headaches respond well to over-the-counter (OTC) medications like ibuprofen or acetaminophen. Lifestyle adjustments, such as improving posture, staying hydrated, and practicing relaxation techniques, often reduce the frequency of these episodes.
For Migraines:
Migraine management is dual-pronged:
- Abortive Treatments: Medications taken at the first sign of an attack to stop the process (e.g., Triptans).
- Preventative Treatments: Medications or therapies taken daily to reduce the frequency and severity of future attacks (e.g., Beta-blockers, anti-seizure meds, or CGRP inhibitors). [Insert Image: Illustration of different medical treatment options for chronic pain]
Recovery and Prevention Tips
Prevention is often the best “cure” for chronic head pain.
- Establish a Routine: Eat and sleep at the same time every day to keep your body’s internal clock stable.
- Stay Hydrated: Dehydration is a subtle but powerful trigger for many.
- Manage Stress: Techniques like yoga, meditation, and deep breathing can lower the physiological triggers of pain.
- Limit Caffeine: While a little caffeine can help a headache, “rebound” headaches occur when you consume too much or quit abruptly.
- Regular Exercise: Consistent, moderate exercise can reduce the frequency of attacks over time.
Risks and Complications
Ignoring chronic migraines can lead to complications beyond just pain. Chronic migraine sufferers are at a higher risk for depression, anxiety, and sleep disorders. Furthermore, the over-reliance on OTC painkillers can lead to “medication overuse headaches,” where the medicine itself causes a cycle of chronic pain. If you find yourself taking pain medication more than two days a week, it is a sign that your condition is not being managed correctly and requires expert critical care or neurological consultation.
When to See a Doctor
While most headaches are benign, some require immediate medical attention. You should consult a specialist if:
- The pain is “the worst headache of your life” and comes on suddenly.
- You experience a headache following a head injury.
- Pain is accompanied by a fever, stiff neck, confusion, or seizures.
- Your headache pattern changes significantly or worsens after age 50.
- You have weakness or numbness in any part of your body. Early intervention is key to preventing the progression from episodic to chronic migraine. If you are struggling to manage your symptoms, don’t wait for the next attack. Book an appointment with our experts today to develop a personalized treatment plan.
Conclusion
Distinguishing the difference between migraine and headache is vital for effective treatment. While a headache might be a temporary inconvenience, a migraine is a serious neurological event that demands specialized care. By identifying your triggers and seeking professional help, you can move away from simply “enduring” the pain and start living a life defined by wellness rather than your next attack. At Raj Hospitals, our dedicated team is here to support you with advanced diagnostics and compassionate care. If you’re ready to find a long-term solution for your head pain, consult a specialist today and take the first step toward a pain-free future.
Frequently Asked Questions (FAQs)
Can a regular headache turn into a migraine?
While they are different conditions, frequent tension headaches can sometimes coexist with migraines. However, one does not “evolve” into the other; rather, a person may suffer from both types of primary headache disorders simultaneously.
How long does a typical migraine last?
A migraine attack can last anywhere from 4 hours to 72 hours. Some people may also experience a “migraine hangover” (postdrome) for a day or two after the intense pain has subsided, feeling drained or confused.
Are migraines hereditary?
Yes, genetics play a significant role. If one or both of your parents suffer from migraines, you have a much higher likelihood of developing them yourself.
Is there a permanent cure for migraines?
Currently, there is no permanent cure that eliminates migraines forever, but they can be highly managed. With the right combination of lifestyle changes and modern medications, many patients can reduce their “migraine days” by 70-90%.
Can diet really help in reducing the difference between migraine and headache frequency?
Absolutely. Eliminating trigger foods like MSG, artificial sweeteners, and nitrates, while maintaining stable blood sugar levels through regular meals, is a proven strategy for reducing attack frequency.
Why does my head hurt only on one side?
Unilateral (one-sided) pain is a hallmark characteristic of migraines. It is thought to be related to the activation of the trigeminal nerve on one side of the brain, though the pain can sometimes shift sides in different attacks.











